The use of Flexible Intramedullary Nails has been a game changer in orthopedic surgery. Dr. John Smith, a renowned expert in bone fixation techniques, notes, "These nails provide unmatched stability for fractured bones." Their adaptability makes them suitable for a range of injuries.
Flexible Intramedullary Nails allow for minimal invasiveness. This can lead to faster recovery times. Surgeons value their ability to support complex fractures. However, not all nails are created equal. It is essential to choose the right type for optimal outcomes.
Despite their advantages, some concerns arise. The flexibility might lead to malalignment if not placed correctly. Additionally, surgeons must be cautious about the learning curve associated with these tools. This highlights the importance of training and experience in employing Flexible Intramedullary Nails effectively.
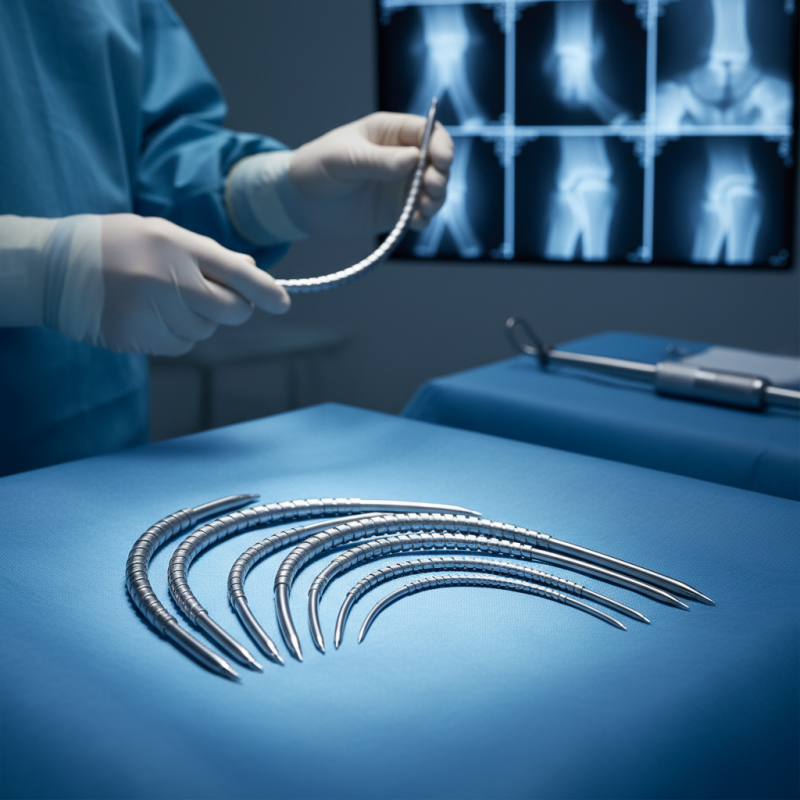
Flexible intramedullary nails play a crucial role in orthopedic surgery. They provide significant support for fractured bones, particularly in children. These nails are useful for stabilizing complex fractures, especially in the long bones of the arms and legs. Surgeons insert them through the medullary cavity, allowing for minimal disruption to surrounding tissues. This technique fosters faster healing.
However, the effectiveness of these nails can vary. One common concern is the risk of improper placement. If not positioned accurately, they may not provide adequate support. Additionally, the patient's anatomy can influence outcomes. In some cases, nails may bend or break, leading to complications. Surgeons need to consider these factors carefully during the procedure.
Recent advances in design have improved the functionality of flexible intramedullary nails. They come in different sizes and shapes, catering to various fracture types. Despite these innovations, challenges remain. Not all surgeons are trained in the latest techniques. This can lead to inconsistent results across different cases. Education and training are essential for improving patient outcomes with this method.
Intramedullary nails are crucial for stabilizing bone fractures. Different materials impact their effectiveness and usability. Titanium is lightweight and strong. It offers excellent biocompatibility but can be costly. Stainless steel is more affordable. It provides durability but may cause increased thermal sensitivity. The choice of material can influence healing time and comfort for patients.
When choosing intramedullary nails for bone support, consider the patient's condition. For example, those with allergies may need alternative materials. On the other hand, heavier individuals might require sturdier nails for effective support. Always discuss potential outcomes with healthcare providers.
Tips: Always prioritize comfort in material selection. Test choices in simulated environments if possible. Don’t overlook how temperature changes can affect the chosen materials. Reflect on the long-term impact of your decision. The right intramedullary nail can lead to successful recovery, but it’s essential to weigh all options carefully.
When it comes to intramedullary nails, mechanical properties are crucial. These nails need to provide adequate stability during the healing process. Load-bearing capacity directly affects recovery times. If a nail can’t support the bone adequately, complications may arise. Issues such as misalignment or delayed healing can occur.
Modern nails are often designed with a combination of materials. Some are more flexible, allowing for better adaptation to bone movements. However, flexibility can also lead to decreased rigidity in certain situations. This trade-off is an area for further research. The ideal balance between flexibility and strength remains to be firmly established.
Another aspect to consider is the surface treatment of nails. A treated surface can enhance attachment and promote bone growth. But what if the treatment affects the nail's overall durability? Such questions are worth exploring. The ongoing development of intramedullary nails is vital for improving outcomes in bone support. Each design brings its own set of advantages and challenges, making this a field ripe for innovation.
Flexible intramedullary nails have emerged as a revolutionary solution for bone support. Their design allows for easy insertion and adapts to the contours of the bone. Many studies highlight significant improvements in healing times. However, results can vary depending on the type of fracture and individual patient factors.
Clinical outcomes show that these nails can enhance stability during recovery. They allow for early mobilization, which may accelerate rehabilitation. Patients often report reduced pain and increased functionality. Yet, there are instances where complications arise. Some patients experience issues like malunion or nonunion. This underscores the importance of careful selection and monitoring during treatment.
Despite the proven advantages, not every case is straightforward. Surgeons should evaluate each situation thoroughly. They must consider factors such as fracture location and patient health. Continuous research is essential to refine techniques and improve outcomes. The journey of bone healing is complex, and flexible nails contribute significantly, but they are not a one-size-fits-all solution.
| Material | Diameter (mm) | Weight Bearing Status | Healing Time (Weeks) | Complication Rate (%) |
|---|---|---|---|---|
| Titanium | 8 | Full Weight Bearing | 6 | 5 |
| Stainless Steel | 7 | Partial Weight Bearing | 8 | 8 |
| Carbon Fiber | 6 | Full Weight Bearing | 5 | 3 |
| Composite Material | 9 | Full Weight Bearing | 7 | 6 |
| Bio-resorbable | 8 | Partial Weight Bearing | 9 | 10 |
Intramedullary nails have advanced significantly. Recent innovations focus on enhancing bone support during healing. New designs offer flexibility and strength, which helps to reduce the risk of complications. Surgeons can now choose tailored options for diverse fractures. Materials used are lighter yet robust. These changes can significantly improve patient outcomes.
One exciting development is the introduction of interlocking features. This allows for better stabilization of the bone. Patients often express relief when they learn about these improvements. However, the learning curve for some surgeons remains a challenge. Transitioning to these new designs requires time and practice. There's a need for comprehensive training programs.
Another aspect to consider is the range of motion. Some designs permit more natural movement during recovery. This can be a double-edged sword. While beneficial, it may lead to discomfort for some patients. Understanding individual needs is critical. The goal is to find the right balance between mobility and stability. Each patient’s journey is unique and requires careful attention.